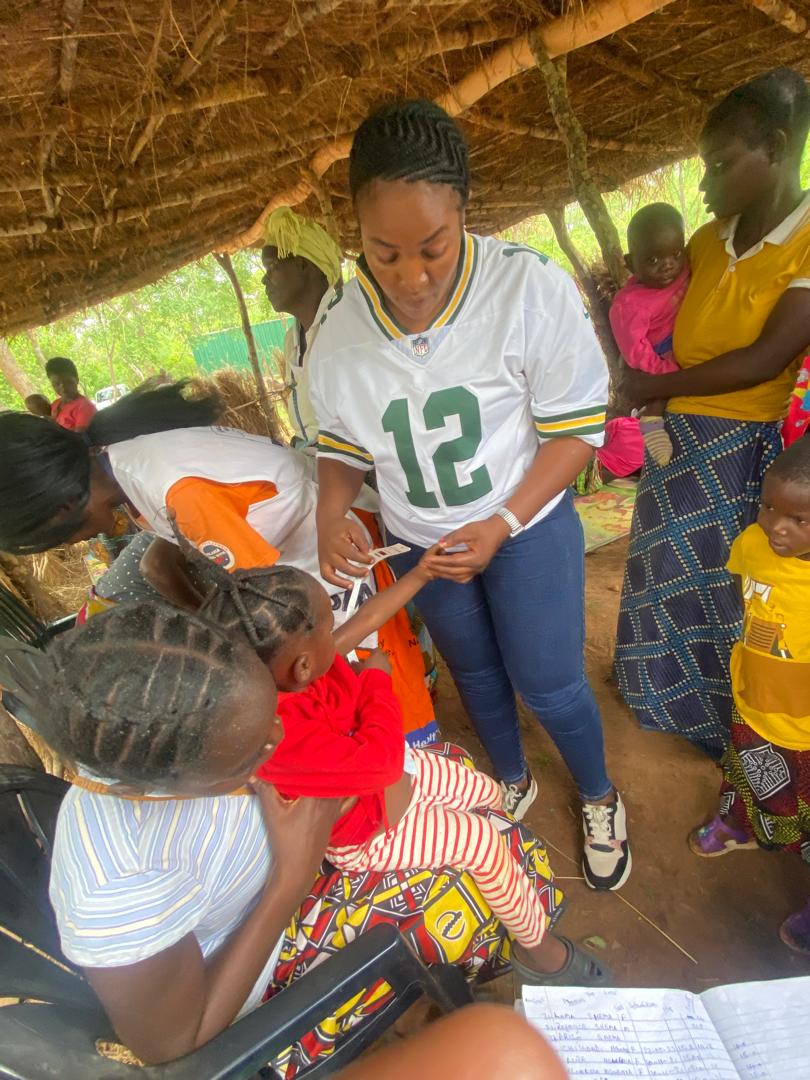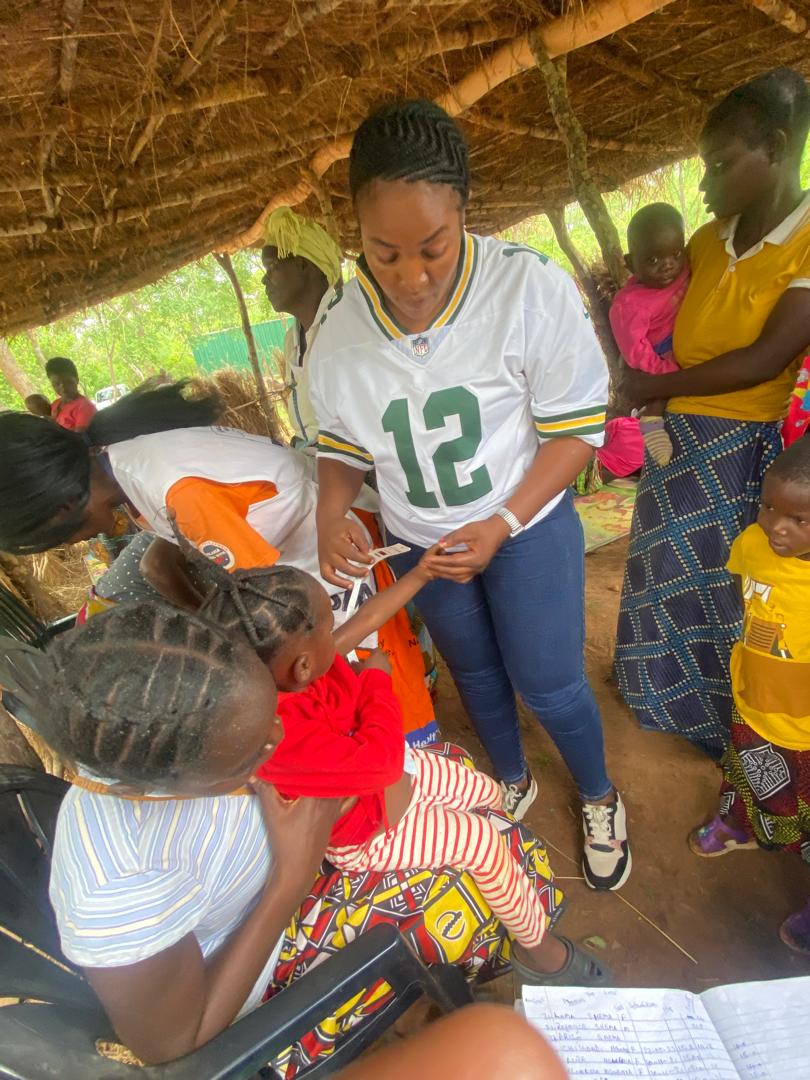





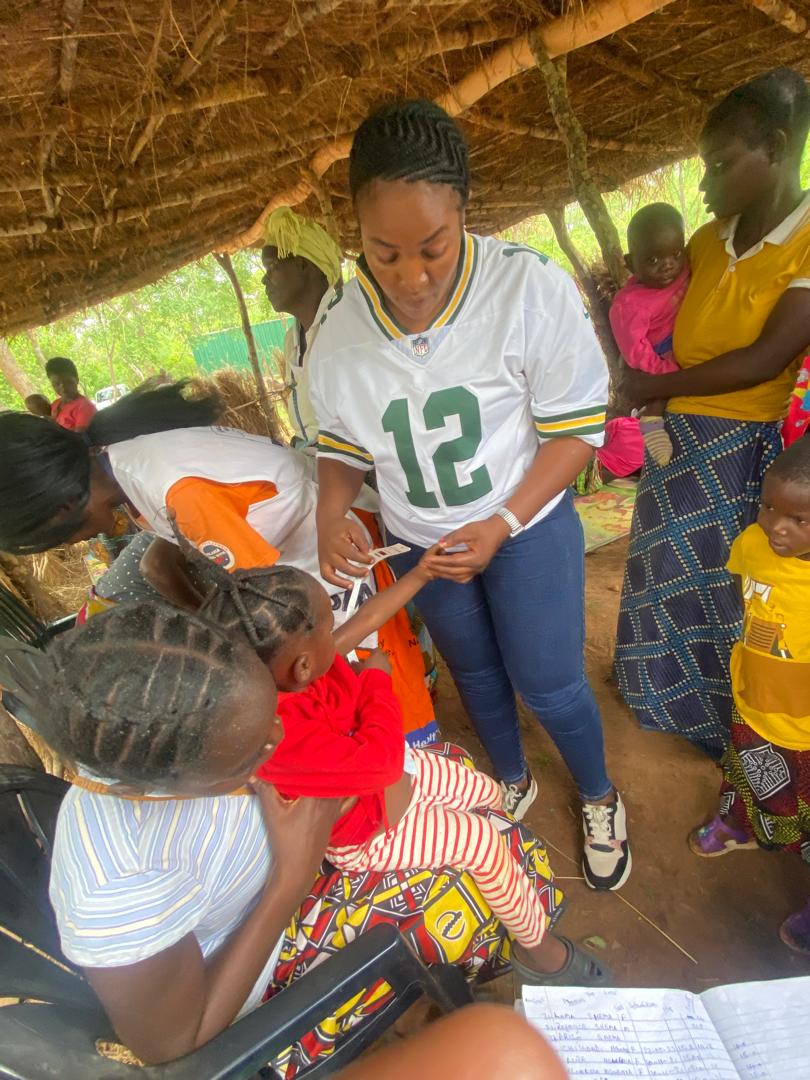



Report on Women's Activity Under Women's Federation
Date: 5th December 2025
Location: Hyojeong Center, Mishoro Village , Chipata, Kasenegwa district, Eastern Province, Zambia
Report Prepared By: Women's Federation Leadership
Status: Critical - Escalation of Severe Malnutrition Cases
1.0 Executive Summary
The December session underscored a critical shift towards formalized collaboration with district health authorities, facilitating advanced health monitoring. However, the data collected revealed a deeply alarming escalation in child malnutrition. The identification of 10 children with severe acute malnutrition (SAM) necessitated an immediate change in protocol, while severe weather highlighted the program's infrastructural vulnerabilities, disrupting crucial activities.
2.0 Attendance & Official Delegation
• Mothers Present:116
• Children Present: 146
• District Nutrition Team: Mrs. Linda Zangi (District Nutritionist), accompanied by two volunteers, Mrs. Agnes Zulu and Forri.
3.0 Activity Breakdown & Integrated Workflow
The session demonstrated an effective multi-tasking model with distinct, simultaneous stations:
1. Nutrition Demonstration (Led by Mrs. Severine Lupili): Continued practical education on preparing soya porridge.
2. Maternal Education (Led by Mrs. Linda Zangi): A comprehensive 1-hour 15-minute session focused on antenatal and newborn care, expanding the educational scope from child nutrition to maternal health.
3. Child Registration (Led by Mrs. Florence Chanda): Systematic logging of children's names for accurate record-keeping.
4. Anthropometric Assessment (Led by Volunteers): Mrs. Agnes Zulu and Forri conducted precise measurements of children's height and weight. Mrs. Zangi utilized a specialized tape measure for Mid-Upper Arm Circumference (MUAC), the standard tool for diagnosing severe acute malnutrition.
4.0 Critical Findings: Severe Acute Malnutrition (SAM) Crisis
The professional assessment confirmed a serious health emergency:
• Newly Identified Cases: 6 children diagnosed with SAM.
• Referred Cases to the Clinic: 4 children with SAM.
• Total SAM Cases Requiring Urgent Intervention: 10 children.
Professional Directive from Mrs. Linda Zangi: Given the severity, she mandated the creation of a separate, dedicated program for these children. This must include:
• Specialized Cooking: Preparation of energy-dense, therapeutic foods.
• Targeted Counseling: Intensive nutritional counseling and support for their caregivers.
5.0 Logistical Disruption
The session was prematurely concluded due to a
heavy rainfall. The lack of adequate, permanent shelter prevented the continuation of activities, including the vital planning for the new SAM program and further maternal counseling. This incident starkly illustrates how environmental factors and infrastructure deficits directly hinder healthcare delivery.
6.0 Analysis and Implications
1. Partnership Success: The active, on-ground involvement of the District Nutritionist represents a significant achievement in formalizing support.
2. Deepening Health Crisis: The identification of 10 SAM cases is the most severe reported to date. It validates previous concerns and indicates that the general porridge program, while beneficial for moderate malnutrition, is insufficient for the most critical cases.
3. Systematic Approach Introduced: The use of MUAC tapes and the directive for a separate SAM feeding program aligns with national and global health protocols, marking a necessary transition to more professionalized care.
4. Infrastructure as a Critical Barrier: The weather-related disruption is not a minor inconvenience but a major barrier to consistent care, especially for critically ill children who cannot miss sessions.
7.0 Urgent Recommendations and Next Steps
1. Immediate Medical Action: The 10 SAM cases must be referred immediately to a clinical stabilization center or an outpatient therapeutic program (OTP) as per national guidelines. The district team's involvement should facilitate this referral.
2. Establish SAM Program: Work with Mrs. Linda Zangi to urgently establish the separate feeding and counseling group for SAM children, securing the necessary therapeutic food supplies.
3. Emergency Shelter Solution: Prioritize the construction or procurement of a large, weatherproof tent or permanent shelter as a non-negotiable requirement for program continuity and child safety.
4. Data-Driven Planning: Use the collected height, weight, and MUAC data to formally categorize all children: Green (Healthy), Yellow (Moderate Malnutrition), Red (SAM), to tailor interventions precisely.
5. Follow-up Communication: Draft a formal report of the findings (including the 10 SAM cases) to the District Health Office, requesting concrete support for the SAM program and infrastructure.
8.0 Conclusion
December's session was a watershed moment, moving from anecdotal observation to professional diagnosis. The partnership with district health authorities has revealed the true, grave scale of the malnutrition crisis. While this is sobering, it provides the clear evidence needed to mobilize targeted, life-saving resources. *The immediate focus must now split between continuing general support and launching an emergency intervention for the 10 most vulnerable children.* The program's ability to adapt to this new reality is its most critical test.
Next Scheduled Session: 2026
Proposed Focus: Launch of SAM Therapeutic Feeding Program & Shelter Solutions.